- Author:
- Rajendra Chavan, Suzana Loshkovska
- Subject:
- Health, Medicine and Nursing, Social Work
- Material Type:
- Full Course
- Level:
- Community College / Lower Division, College / Upper Division, Adult Education
- Tags:
- License:
- Creative Commons Attribution
- Language:
- English
- Media Formats:
- Downloadable docs, Interactive, Mobile, Text/HTML
Claude Bernard
DCCT Trial 1993
google classroom-monitoring-diabetes-hypertension
IDF Diabetes Atlas
Kids and diabetes in schools by IDF
Oxygen saturation
UKPDS
Using a digital BP monitor
Using a mercury BP monitor
Using glucometer
WHO Constitution
Monitoring diabetes and hypertension
Overview
The course seeks to familiarize the learners with the possibilities involved in the management of diabetes and hypertension. This course is to make medical knowledge simpler and accessible for common people. This will help reduce anxiety about the diseases. Reduction in the incidence of threatening complications like cerebral stroke, heart attack, kidney failure, blindness, diabetic foot and amputations is the goal we need to achieve.
The health-aware person, a learner of this course, can be a patient itself, a relative, a neighbor, or anyone from society. Some basic education and a will to help the patient is all that is required.
Abstract
The central idea of this course is that a trained voluntary health-literate can assist doctors in diagnosing, monitoring, and treating people with diabetes and hypertension. One simple test, one small observation, one timely consultation by the volunteer can prevent dreadful moments for the patient.
This health-aware person, a learner of this course, could be a patient himself or herself, a relative, a neighbor, or anyone from society. Some basic education and a will to help the patient is all that is required.
Diabetes and hypertension are quite prevalent globally.
Global diabetes data report 2010 — 2045
With a large number of patients, it is getting difficult for the present healthcare systems to reach every patient in need of medical intervention. Especially in rural areas and where traveling is still a difficult task, where people are unwilling (for a variety of reasons) to visit a doctor frequently, where there are fewer doctors as compared to the population, such as in India.
Nearly every family has a patient with hypertension, diabetes, or both. Many patients remain undiagnosed because they are asymptomatic many times.
This course seeks to familiarize the learners with the possibilities involved in their role in the management of diabetes and hypertension. The goal of this course is to make medical knowledge simpler and accessible for common people. This will help not only demystify these diseases but also reduce the anxiety about them. Reduction in the incidence of serious and life-threatening complications like cerebral stroke, heart attack, kidney failure, blindness, and diabetic foot and amputations is the goal we need to achieve.
Introduction
Background
The thought behind this course Fear of the disease is mostly due to ignorance. Knowledge is the answer. This is an attempt to do that. People just know the names of diseases but that is not enough. They should gather enough information and live a fear-free life. |
I have a clinic in a village in Konkan, the western part of Maharashtra state in India, where I have been treating diabetes and hypertension patients for the last forty years. In these years, I have learned that there is no alternative to close monitoring of blood sugar and blood pressure for adequate management of diabetes and hypertension. However, most of the time, people around are not educated enough or health-literate to monitor themselves or their family members.
I thought of the above fifteen teenagers of these families. These young students were studying in schools or junior colleges. They already have some health lessons in their curriculum. It was the right time to make them aware of these prevalent diseases. Due to the theatre activities, I am connected to most of the students in the school. So I began a dialogue with them about a project I had in my mind.
I often thought that how lucky are people when they have a doctor in their family. It is really not possible but we can at least have someone who has learned some skills in medicine and has read enough information to guide the family members.
When an elder member in a family is sick everyone is worried. Though they want to help the person they do not know how to do that. If they learn a few medical skills like using a thermometer, measuring a pulse rate, and respiratory rate. They can learn the basics of wound care easily. Using the Blood pressure apparatus is also not a big thing to do. If explained well they can even measure blood glucose with a glucometer. I wanted to make them health-literate as early as possible.
I went to the school in our village and explained the idea to the school authorities and we started Saturday and Sunday discussion sessions with the interested students. We had ten sessions of one hour each. We discussed health and illnesses in general. Diabetes and hypertension were discussed in detail. We learned together to measure blood pressure, feel the pulse, and use a glucometer.
Then, we arranged a camp for diabetes and hypertension for people in the area with the help of these volunteer students. Diagnosis and guidance were the aims. We repeated this activity with different batches of students for the next three years.
These camps were helpful for people. We detected many new cases and could arrange discussion sessions for all new and old patients. Every camp was attended by more than three hundred people; three to four camps in a year. There were around thirty volunteer students who took blood pressure and measured blood sugar under the supervision of volunteer doctors in the village. We held an open discussion among doctors in the village who shared their experiences about the management of diabetes and hypertension in the camps in front of the patients. There was a question-answer session with the audience after the discussion.
We had named this activity ‘school for health’. The present course is an online version of this particular thought. Problem-oriented discussions among the participants will enhance group learning.
Diabetes and hypertension
As silent killer diseases
Diabetes and hypertension are called silent killers.
This means that they can lead to complications causing sudden deaths without any preceding symptoms. This is unique to diabetes and hypertension. Undiagnosed and borderline diseases cause irreversible damage to organs. People remain unaware of the disease that exists within their bodies. They don’t consult a doctor as they do not have a troublesome, recognizable symptom.
Dyslipidemia or increased fats in the blood is another such modern human disease. These are all chronic acquired diseases also listed under the broad name of non-communicable diseases.
Another term used is lifestyle diseases.
We observe heart attacks, cerebral strokes, kidney failures, retinal detachments, ketoacidosis, non-healing wounds, and gangrenes. But we miss the hidden culprits sitting under. Those are long-standing untreated hypertension and hyperglycemia. Those are diabetes and hypertension. They remain the fastest-growing public health issue for the last forty years or so.
The reasons are many. And not all have yet been identified or well-understood. Changed dietary habits, physical inactivity, and stress create the ground for these diseases. And hence there is a need for a different approach to deal with them. Frequent examinations for blood glucose and blood pressure levels are required with a continuous suspicious mind to know if someone is suffering from diabetes or hypertension. And if someone is not being treated adequately.
Medicine has a long history to overcome diseases
Time brings us here and we are to decide about our future with thoughtful actions. Education, communication, and collective actions have always helped us to survive and get through difficult situations till now.
How we think about the cause of a disease has kept changing with time. Many scientists work hard over their lifetimes to find out the facts. Every disease is investigated and the cause is identified. The treatment is sorted out. And we get rid of the problem. We have gotten rid of many diseases till now. Science has got a methodology to deal with diseases.
Knowledge on a fingertip
We are now in the era of the internet. We have vast amounts of information in every field of life. It is at our fingertips, just a click away from every person with an internet connection. The internet and mobile technology are spreading rapidly in every country. Now it has become easier to reach people and communicate. Open education for a better world (OE4BW) is one such kind of momentum. This resource is part of it.
Scientific mind at work
Not all people living at a particular time have the same opinion about a particular subject.
Diabetes and hypertension are not an exception. Education and discussions make the difference. Research should reach people. The patient should follow evidence-based medicine. Small attention is required to know the exact reason behind the suffering. Armed with this knowledge, it is easily possible to stay fit and healthy despite the disease.
Health is wealth
Prevention is the best cure they say. Early diagnosis and proper care are almost like a cure.
Diabetes and hypertension are to some extent preventable diseases. Since we know the risk factors involved we can avoid them. We aim to prevent complications. If complications are treated well we can prevent disabilities.
The present course about monitoring blood glucose and blood pressure is important as a preventive measure at every stage of the disease. Monitoring will prevent repeated hospitalizations. Monitoring will reduce the economic burden due to these chronic diseases.
The course structure
We have divided the course into three modules.
Module 1
The Disease:
Module 2
The patient
Module 3
The monitoring
Restrictions: Knowing the limitations as a volunteer/mediator
Response: Self-assessment of the work
Reaching:: Building the network of voluntary health literates
Research: Comparative study if possible
Module 1 The Disease: The concept of health and disease
Module 1
Diabetes and Hypertension
The concept of health and disease
Life is like a river flowing continuously without a moment of rest. We grow old with every heartbeat. Cells die and newer ones take their place. We are unaware of many minute happenings that take place in our bodies. We are unaware of the working of our minds. The chemical reactions take place throughout the body and messages travel from place to place with the speed of the electric current. The functioning of the body is not noticed by us. We are not disturbed by our bodies most of the time. I think that is what happens when we are in good health. The smooth functioning of our body systems has an ultimate feeling of health to us. Health is the well-being of the mind and that of the body.
“Health is a state of complete physical, mental and social well-being and not merely the absence of disease or infirmity” – WHO Constitution |
This WHO definition of health, dated back to 1948 is still valid today. It covers the health of mind, body, and our interaction with the society we live in.
Health for all by 2020
Total health is difficult to attain in today’s world. Healthy individuals together will make a healthy society. Hence we had thought of ‘Health for all by 2020’. And now we have already missed that deadline.
Unfortunately, the pandemic of Covid-19 has taken away the little progress if at all we had made by 2020. The world is affected badly today. We were not prepared for this calamity. Uncertainty is ruling the world it seems. That should not dishearten us and we must prepare ourselves and improve our capacity to reach our goal of health for all.
We have witnessed that diabetes and hypertension are making it difficult to fight the virus. Covid-19 is more lethal when an infected person has these comorbidities.
Diabetes and hypertension monitoring has become so important in the present situation.
Life with the disease is bound to be different. But we can help make it bearable, painless, and full of hopes and dreams. Even talking for a few minutes and listening to their experiences is going to help the patients. Here, we are trying to help them, understand the disease well and make timely decisions to maintain their health.
Diabetes and hypertension monitored well are as good as no disease. Keeping the glucose levels and blood pressure in the normal range is all that is necessary. |
Module 1 The Disease: Anatomy
Why study anatomy?
It is like viewing a map to plan a trip. It gives the idea of the locations and their relations to each other.
It is the theatre where the play named `life' is performed. If we want to know about life in health and disease we need to go to the place where every action takes place.
Many people have fear or even a nauseating feeling when they look at blood or wounds. It is a natural response for them. One has to overcome this with an intention to go ahead and study an important subject like anatomy. I think the learner of this course is courageous enough to visualize dissected body parts, not the real ones but in pictures, and learn the science of life.
If we want to study diseases and to know about the functioning of our body, then we need to study anatomy. We should know their relations, positions, and importance. We must appreciate the wonderful design of our bodies. How organs are protected by a bony cage is surprising. How muscles function and perform an activity is amazing. One must note the textures, colours, and shapes of various body parts as a student of medicine. The learner here is being introduced to the world of medicine. Anatomy, physiology, and biochemistry are the subjects at the entrance of this world.
Doctors learn anatomy to start the course of medicine after admission into medical college. In the dissection hall, they study cadavers. They dissect bodies to observe and handle bones, muscles, arteries, veins, nerves, tissues, organs. Later on, as a surgeon, they have to know the minute details of the human body as a part of their work.
Nowadays we can visualize internal organs in films of CT scans, MRI, etc. We can learn to some extent with pictures and videos on the internet too. Animation has helped to make simulations and the study of anatomy quite interesting. You can explore the internet to study anatomy whenever you like.
What is our body made up of?
A cell is a building unit of the human body. There are many types of cells and together they give the shape and structure to the body. Cells divide and redivide to form our bodies. It is surprising to see how the life of mankind starts with a single cell. The size achieved in the uterus till birth and its growth afterward are just because of repeated divisions of cells. How cells get differentiated and form tissues, organs, and systems inside the uterus are studied in embryology.
The three-layered embryo turns into a fetus
Initially, the cell divides and forms three layers of the embryo: ectoderm, mesoderm, and endoderm.
The ectoderm forms cells of skin and nails, brain and spinal cord, eyes, epithelium of mouth, nose, and anus.
Endoderm forms cells of the inner lining of the digestive tract and the respiratory tract, and glands, liver, and pancreas.
Mesoderm forms cells of muscles, the circulatory system, kidneys, ureter, bladder, and urethra.
What does every cell do?
Though cells differ in shape and size for different functions, they all have an outer cell membrane and a nucleus inside. They have an intracellular fluid or a cytoplasm. The other structures are nucleolus, mitochondria, endoplasmic reticulum, ribosomes, vacuoles, lysosomes, etc. They together are called organelles. They all together carry on functions of the cell.
Functions of a cell can be listed as:
Structure and support of the body.
Growth by the process of division
Passive transport across the cell membrane, e. g. Oxygen, carbon dioxide, alcohol
Active transport across the cell membrane e.g. bigger molecules like glucose, proteins, polysaccharides
Energy production by process of respiration
Metabolism: includes catabolic reactions, which are breaking bigger molecules.
Anabolic reactions are constructing bigger molecules
from smaller components.
Reproduction: cells take part in the process of reproduction.
It can be mitotic or meiotic division.
Systems of our body and their functions
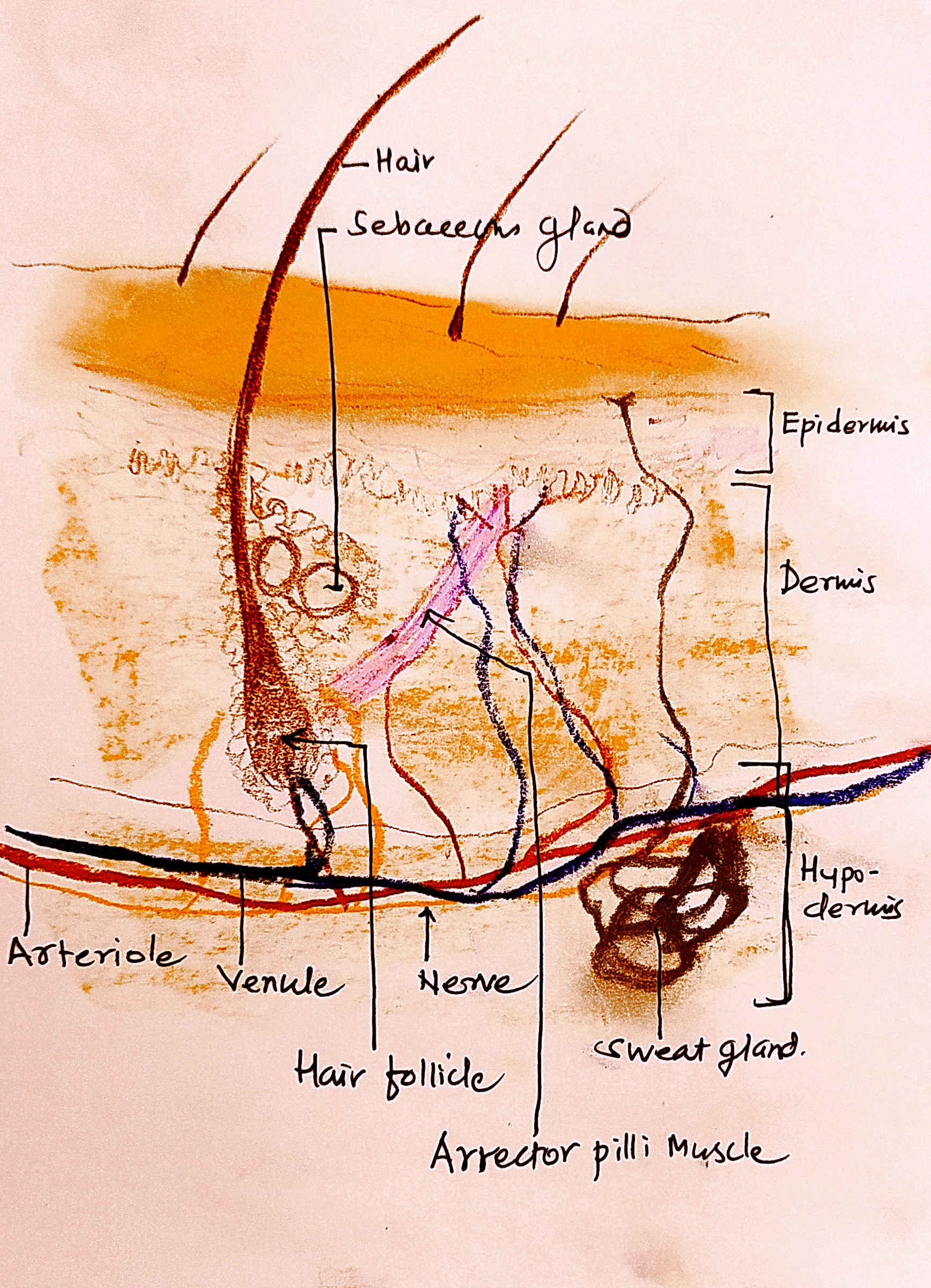
1. skin, hair, and nails
| fig.1 Skin |
Skin is our largest organ. It weighs 4 kg and has an area of about two square meters.
Skin not only covers us but does many functions. Any injury to the skin exposes our body to the possibility of infection by microorganisms. Wound care is a very important part of health care. Every person should learn the techniques of dressing wounds and practice them whenever needed.
Protection
Sensation
Excretion/sweat,sebum
Temperature regulation
Vitamin D production using sunlight
2. Skeletal: skull, spine, shoulder, and pelvic girdles, thoracic cage, hands, and feet bones.
| Fig,2 Skeleton |
Skeleton is used as a symbol of fear in movies. It is also linked with the idea of ghosts.
Recognizing the bones is easy if you observe them for their shape and size. People can find some differences between male and female skeletons. Women have a wider pelvis. Less prominent brows and equally less prominent muscle attachment markings over bones.
Skeleton provides the following functions:
The shape of the body is due to the skeleton.
It supports all other organs/bears weight of the body
Protection for soft organs: the skull protects the brain, ribs protect the heart and lungs
Place of muscle attachment
Joints help in locomotion
Producing blood cells
3. muscular
| Fig.3 Muscles in back as an example |
Locomotion
Work
flexibility
4. nervous: brain, spinal cord, peripheral nerves, sympathetic and parasympathetic nerves
| fig.4 Nervous System |
Controlling the other systems
Interacting with the surroundings
5.respiratory: nose, nasopharynx, pharynx, larynx, trachea, bronchi, lungs
| fig.5 Respiratory System |
Breathing air in and out
Exchange of oxygen and carbon dioxide between air and blood
6.cardiovascular: heart, arteries, veins, arterioles, capillaries
| fig. 6 Cardiovascular System |
- Carry oxygen from lungs to body cells
Carry carbon dioxide from cells to lungs
Carry digested food/nutrients from the digestive system to cells
7.lymphatic: lymphatic vessels, lymph nodes, thymus, tonsils, and spleen
| fig.7 lymphatic system |
Drain the fluid from capillaries to veins
Maintain the balance of extracellular fluid and that in the vessels
Carry immune cells from the immunity system to the body
Spleen destroys old RBCs (red blood corpuscles)
8. digestive: Teeth, tongue, salivary glands, pharynx, esophagus, stomach, duodenum, jejunum, ileum, colon, sigmoid colon, rectum, liver, gallbladder, pancreas.
| fig. 8 |
The figure shows the position of the pancreas
Breaking the food into small size molecules
Excretion of bile and undigested food
The pancreas and liver have various other functions
9. urinary: kidneys, ureters, bladder, urethra
| fig.9 Urinary system |
Filters blood to remove waste
Maintains the blood pressure
10. reproductive: mammary glands, uterus, ovaries, vagina/testes, seminal vesicles, prostate, and penis
| fig.10 Reproductive System |
Reproduction
11. endocrine: pituitary, pineal gland, thyroid, parathyroid, suprarenals, pancreas, testes, /ovaries
| Fig. 11 Endocrine System |
Producing hormones that control other systems
Growth and functioning
Module 1 The Disease: Physiology
Functioning of the human body
Physiology tries to understand how the body functions. It is a branch of biology.
It is learned with so many experiments that biology works with the laws of physics and chemistry.
So, in physiology, we need to go in-depth about the processes involved. Every system needs to be studied from that angle.
What are the functions of our body?
Organization
Metabolism
Responsiveness
Movement
Development / Growth
Reproduction
Physiology of blood sugar and blood pressure regulation
How does a normal person always have his/her fasting blood sugar level in a range of 80 to 120 mg/dl,оr blood pressure systolic<120 and diastolic<80 mm of Hg?
These are the desirable ranges for blood sugar and blood pressure in our bodies.
To understand how blood sugar and blood pressure levels are maintained in their respective range, we need to learn the concept of homeostasis.
Homeostasis
Homeostasis is the stability of the internal environment of the body. This ability of the body to control its interior environment was first explained by the scientist Claude Bernard (recognized as the father of modern physiology). The word he used for that was `milieu interieur’.
https://en.wikipedia.org/wiki/Claude_Bernard
https://www.britannica.com/biography/Claude-Bernard
The body has different systems working separately but all are well connected and are interdependent too. To have an ideal environment for the best functioning of our body some conditions need to be fulfilled. These conditions are many. For example, body temperature, pH of blood, blood sugar, etc. Our body control systems work together for maintaining these values in the desired range. The system acts like that of the thermostat, which maintains the temperature near the set point.
The human body requires energy for functioning. The energy we get is from the food we eat.
Our food is in three main forms. Those are proteins, fats, and carbohydrates. When these three forms are digested they get absorbed into the blood flow as amino acids, fatty acids, and glucose respectively.
Glucose is used to give instant energy. It is easy to understand that blood glucose/sugar is raised when we eat food containing glucose. Carbohydrates are a rich source of glucose. Then glucose molecules enter cells for their further utilization. Here insulin secreted by beta cells of the pancreas is required for the active transport of glucose molecules through the cell membrane. The glucose that enters the cell undergoes glycolysis. This is an irreversible reaction and it gives one ATP molecule. ATP is used as energy throughout the body.
The body has glucose reserves, stored glucose in the form of glycogen. Mostly in the liver and skeletal muscles. This storage process, called glycogenesis, is also promoted by the hormone insulin. The extra glucose, if available, is converted into fats or adipose tissues for long-term storage. When the glucose level starts falling glycogen molecules are again converted to glucose and brought back into blood circulation for utilization. The reaction is the opposite of glycogenesis. So glycogenolysis is breaking down glycogen molecules in small parts. That is glucose. Glycogenolysis = Glycogen+lysis. The hormone which plays a role here is glucagon. Glucagon is secreted by alpha cells of the pancreas. In some situations when required glucagon can produce glucose from proteins too. It is called gluconeogenesis. At the time of starvation, glucagon converts fatty acids to ketone bodies. The process is called ketogenesis. They increase the acidic level of blood and cause a condition known as ketoacidosis.
Role of hormones in the homeostasis of glucose
1. insulin
Insulin reduces blood sugar by
Glycolysis: by helping glucose enter into the cell.
Glycogenesis: by increasing the glucose conversion to glycogen in the liver and muscles.
Lipogenesis: by converting glucose to fats.
2. Glucagon
Glucagon increases blood sugar by
Glycogenolysis: Converts glycogen to glucose
Gluconeogenesis: Converts amino acids to glucose
Glucagon is an exceptional condition of starvation that produces ketone bodies from fats.
Ketone bodies are used instead of glucose as a source of energy only by the brain and heart.
As if this is the last life-saving alternative available to the body.
Ketogenesis: Fats are converted to ketone bodies.
3. Amylin (islet amyloid polypeptide)
Secreted with insulin by beta cells.
Helps to decrease postprandial blood glucose spikes by
Slowing the gastric emptying
Promoting satiety
4. Incretins
GLP-1
GIP
Incretins are hormones secreted by epithelial cells of the small intestine.
The entry of food or glucose triggers the secretion.
They increase insulin release by beta cells of islets of Langerhans in the pancreas. They decrease glucagon secretion. They also delay gastric emptying and promote satiety.
But they are deactivated by the enzyme DPP4 in a short time.
New drugs DPP4 Inhibitors prolong the action of incretins and reduce blood glucose.
Other hormones
5. Growth hormone secreted by the pituitary gland,
6. Cortisol secreted by suprarenal or adrenal glands,
7. Adrenaline by adrenal glands,
All the above three hormones have hyperglycemic effects. Means they increase blood glucose levels.
| fig.12The graph below is blood glucose values against time. |
Module 1 The Disease: Diabetes: Types
Diabetes
What is diabetes?
Diabetes is a metabolic disorder causing raised blood sugar, also known as hyperglycemia.
It occurs due to a deficiency of the hormone insulin. But it can also occur due to the phenomenon of insulin resistance, where insulin is ineffective though not deficient. It is called a relative deficiency of insulin.
Insulin is a hormone produced by beta cells of the islets of Langerhans in the pancreas.
Though diabetes is a metabolic disorder it affects small and large vascular systems, causing inflammation of endothelium (inner walls of the blood vessels). So it is equally a cardiovascular disease. |
Types of diabetes mellitus(DM)
Type1 DM:
Type1 diabetes mellitus was previously known as Insulin Dependent Diabetes Mellitus, (IDDM).
It starts early in life and children suffer from this, hence is called juvenile diabetes too. This type of diabetes is due to the autoimmune destruction of beta cells in islets of Langerhans of the pancreas. Autoimmunity is when our immune system fails to recognize our cells and produces antibodies against our own cells.
Destroyed and non-functioning beta cells lead to worrisome conditions for Type1 DM patients as they do not have endogenous insulin to control their blood sugar. If not treated the sugar is too high and causes complications like ketoacidosis and sometimes altered consciousness. The patients can still lead a good life when treated properly with insulin. The life span and the quality of life are improved after insulin treatment. Insulin has saved many lives.
To learn more about juvenile diabetes it is worth visiting the sites below.
Type2 DM:
Type2 diabetes mellitus was previously known as non-insulin-dependent diabetes mellitus(NIDDM). It starts mostly after forty years of age and is also called maturity-onset diabetes. As some insulin is produced this diabetes remains asymptomatic for a longer duration.
It is due to the dysfunction of beta cells of islets of Langerhans in the pancreas and associated insulin resistance. Type2 DM is the commonest type of diabetes. Nearly 90 percent of total diabetics have Type2 DM.
In this course, we are mostly dealing with this type of diabetes.
Gestational diabetes
This type of diabetes is found in some of the expecting mothers (around 2-3 percent) during the
last trimester mostly. The cause here is insulin resistance. This hyperglycemia reduces on its own after the delivery.
Pancreatic diabetes
The main cause here is repeated and chronic pancreatitis. Due to inflammation, the pancreatic tissue is destroyed. There are fibrotic lesions and calcifications in the pancreas. Both exocrine and endocrine functions get affected. The patients have upper abdominal pain and indigestion in association with hyperglycemia. This type of diabetes is difficult to treat as the sugar levels always keep fluctuating. The patients remain malnourished. But monitoring blood sugar is essential to reduce possibilities of hypoglycemia or hyperglycemia.
Comparison of Type1 DM to Type 2 DM
| T1DM | T2DM | ||
Juvenile diabetes mellitus |
| ||
| Starts in childhood | Starts after age 40 usually | ||
| Symptoms are acute | symptoms develop gradually | ||
| The patient is usually thin | The patient is usually obese | ||
| Need insulin in the treatment | Insulin may be needed | ||
| Can not be prevented | Risk is reducible |
Module 1 The Disease: Diabetes: Symptoms
Symptoms of diabetes
Symptoms depend on the level of hyperglycemia. If the blood sugar is below 180mg/dl then the patient may not have any symptoms, that is the patient is asymptomatic.
As we know now, hyperglycemia is a raised blood glucose level. When the blood glucose is more than 180 mg/dl it crosses the renal threshold. Meaning the kidney starts excreting glucose through urine. Normally glucose is nil or is absent in urine. If glucose passes the kidney’s barrier it pulls the amount of water in its proportion by the laws of osmosis. A large quantity of water passes with glucose in urine. This causes dehydration. Cells experience dryness which stimulates the thirst center. The person feels thirsty quite often. As insulin shortage or insulin resistance causes few glucose molecules to enter cells, cells lack the energy source and are starved. This causes hunger. Sugar in urine invites infection by fungi.
Polyuria: passing large amounts of urine, frequently.
Polydipsia: Increased thirst
Polyphagia: Increased appetite.
Glycosuria: Passing glucose in urine.
Unexplained weight loss
Fatigue
Irritability
Delayed wound healing
Blurred vision
Frequent infections
Module 1 The Disease: Diabetes: Diagnosis
Diagnosis of diabetes
( Patient's serum mixed with the reagent in a laboratory)
If the person has symptoms mentioned above, s/he is investigated further. If s/he has blood tests done twice at an interval positive, s/he is considered to have diabetes. The tests performed are as follows:
Fasting plasma glucose (FPG)
(Fasting means no caloric intake for eight hours.)
FPG ≥ 126mg/dL
OR
Oral glucose tolerance test (OGTT)/2- Hour plasma glucose(PG)
(Patient is given 75-gram anhydrous glucose dissolved in water 2 hours before the test)
2-hour PG ≥ 200mg/dL
OR
HbA1c ≥ 6.5%
OR
If the patient has classic symptoms of hyperglycemia then
Random plasma glucose ≥ 200 mg/dL
Prediabetes
It is when the individual has high blood sugar levels but not so high to be diagnosed as diabetes. Here the fasting sugar will be 100 mg/dL to 125 mg/dL or the postprandial between 140 mg/dL to 199 mg/dL.
This is just a warning sign that the person may have the disease very soon. A healthy and stress-free lifestyle can change the picture. The onset of diabetes can be prevented by dietary changes and increasing physical activity. Jogging, brisk walking, and aerobics are good, proven exercises. Keeping the mind relaxed will also help reduce elevated blood glucose levels.
Glycosylated hemoglobin/ HbA1c
HbA1c is glycosylated hemoglobin. When blood glucose increases some glucose molecules get attached to hemoglobin molecules. This is in proportion to the rise in glucose concentration.
This property of glucose binding to the Hb molecule is used here to see the glucose behavior for the last three months. HbA1c is helpful to guide us about chronic hyperglycemia. Chronic is for a longer duration. The reading of HbA1c gives an idea about the estimated average blood glucose of the last three months.
One millimole of glucose is 18 mg of glucose
HbA1c report estimated average blood sugar in mg/dL & mmol/dL
HbA1C % 5 6 7 8 9 10 11 12 | mg/dL 97 126 154 183 212 240 269 298 | mmol/L 5.4 7.0 8.6 10.2 11.8 13.4 14.9 16.5 |
Other investigations
Once diagnosed the patient needs to be further evaluated to see his/her status regarding possible ill effects due to the disease. They have different symptoms. Their systems get ill at a different pace. It will depend on how long s/he has hyperglycemia and his dietary habits. It will also depend on his/her body mass index and whether s/he has hypertension. Smoking and tobacco chewing and alcohol are worrisome addictions that can exacerbate diabetes.
Urine examinations
Previously we used to use urine examination for monitoring and to diagnose too.
I remember doing Benedict's test in my college forty years back. The color of Benedict’s solution would change from blue to green to yellow to brick red. This was bedside clinical laboratory work for the medical students. The more the sugar, the more the color changes. It was routine work and we used to change the drug dosages depending on the results.
But with the introduction of glucometers, a drop of blood gives results in a few seconds. But still, dry strips for glucose and ketone bodies are useful.
(Diasticks) They have replaced Benedict’s test.
Urine for microalbuminuria helps us judge the beginning of kidneys getting affected. Urinary tract infections are common in diabetics. The pus cells in the routine urine test indicate that.
Lipid profile
Dyslipidemia, when present, adds to the complications. The readings about cholesterol, triglycerides, and the proportion of high density and low-density lipids
provide important information about the state/degree of atherosclerosis we expect.
Serum creatinine
To check and see if any renal impairment has begun. Diabetic nephropathy is a common complication. It is aggravated if associated with uncontrolled hypertension. If Nephropathy is present then the treatment needs to be changed accordingly. Drugs are used with precautions.
Ophthalmic check-up
The patient’s vision needs regular checkups if diabetic. Retinopathy and related blindness are avoidable only with good glycemic control. Long-standing hyperglycemia is also connected to cataracts and optic neuritis.
Cardiac check-up
A basic reading of electrocardiogram gives many clues for patient’s
Cardiac status. Rate, rhythm, conduction of electric current, condition of atria and ventricles, and ischemic changes if any are detected.
Module 1 The Disease: Diabetes: Treatment
There are five parts in the management of diabetes mellitus:
- Patient education,
- Diet,
- Exercise
- Drug treatment
- Monitoring
This is applicable to every disease. But in diabetes, the other parts are equally or more important than the drug treatment. Diabetes being a lifelong companion needs continuous attention. Suppression of the disease is the key to success!
People are claiming that they can even exclude the drug treatment if concentrated enough on diet and exercise. The reversal of diabetes is a popular term used in recent times. It is based on these assumptions and there are many stories available on the internet. It will be a great victory if people get free of the disease without the drugs.
But the day has not yet arrived. What we see is people with complications and difficulties beyond their capacity. Sufferings and economic burdens both are on the rise. Diabetes and other diseases combine to make the solutions difficult. We have observed this with wound sepsis, tuberculosis, AIDS, Urinary tract infections, Atherosclerotic vascular diseases, and many more. The Covid 19 is a recent example.
Patient education
The skill to deal with diabetes is a must for every diabetic. The patient has to know what exactly is the cause and process behind his/her suffering. Informing the patient about diet, exercise, drug dosages, possible side effects is essential. Recognizing the symptoms of hypoglycemia and hyperglycemia is very important.
As the knowledge is ever-changing, updating from experts, magazines should continue.
But the diabetic has to keep away from false advertisements.
Diet
There is a famous term heard often as a diabetic diet. It is a constant fear amongst patients about the diet. People are accustomed to many things in their diet. They have developed the taste over the years from childhood and have developed their formula for eating. Suddenly if they know that they have to restrict themselves to a particular type of food they find the idea difficult.
Diabetes demands meticulous planning in diet. Proper diet to get into the right zone of body mass index, the right blood sugar, and to fulfill the energy demand of the body. A diet should be full of vitamins, healthy nutrients, fruits, and enough fiber.
The doctor treating patients often sends patients to a dietician for proper advice. The dietician takes into consideration the present diet received by the patient, his/her health issues, and the goals of the treatment. The dietician designs meal plans accordingly.
Exercise
The importance and benefits of physical activity have proved beyond doubt now. The lack of physical activity is the leading cause of lifestyle diseases. Simple brisk walking for an hour a day can make a difference. Sedentary behavior is a new urban problem.Household chores, cleaning, gardening, etc. are forgotten. Reduction in this sedentarism and promoting outdoor activities will help a lot.
Being physically active is found to improve insulin sensitivity. It also helps to control blood sugar levels and reduce the average sugar in HbA1c. Altering the dose of insulin and hypoglycemic drugs according to your activity variations is not to be forgotten. The tight control might precipitate hypoglycemia.
Age-related diseases like osteoarthritis affect knee joints and people get into trouble and can not walk for a long time. Frozen shoulders are common in diabetes. Such specific health issues need special attention while treating diabetes.
Hundred years of insulin
Difficult were days for diabetes patients, especially Type 1 DM, before Insulin. Death was inevitable. Starvation was the only treatment known. Diagnosis of Type1 DM was like a death
sentence for the patient.
Frederick G. Banting and Charles H. Best, John J. R. Macleod, and James B. Collip together made it possible to effectively treat diabetes with purified pancreatic extract named insulin. It has proved a life-saving drug for people with diabetes since then. It is essential to know about this discovery but it is important to know how difficult it is for a patient with average income to get treated with insulin.
Insulin is the only drug for Type 1DM. The dosages are based on readings of blood sugar and need constant titration. As insulin is a peptide, if taken orally it is broken down into amino acids and becomes ineffective. Hence it is effective in the injectable form.
Insulin is advised for
Type 1 DM patients
Uncontrolled sugar in Type 2DM even with high dosages of drugs
Type 2 DM with severe infection, cardiac event, or planned surgery
Type 2 DM who needs steroid treatment
Patient with ketoacidosis
Severe hyperglycemia/patient in comatose condition (blood glucose > 600mg/dL)
Short term period insulin for gestational diabetes patient
If the Type 2 DM is allergic to oral hypoglycemic drugs
Patient with diabetes who is only on intravenous support/ no oral feeding
Action duration | Name | Starts action | Peak of action | End of action |
Rapid | Lispro Aspart Glulisine | 5 to 15 minutes | 30 to 90 minutes | 3 to 5 hours |
Short | Regular | 30 to 60 minutes | 2 to 3 hours | 5 to 8 hours |
Intermediate | Isophane (N.P.H.) | 2 to 4 hours | 4 to 10 hours | 10 to 16 hours |
Long | Glargine Detemir Degludec | 2 to 4 hours | No peak hours | 16 to 24 hours |
The type of insulin and the dose and time to inject change according to the response of the patient to the treatment. It is to be remembered that the regimen of drugs or insulin is not likely to work permanently for any patient. The regimens can be once a day, twice a day, thrice a day, four times a day as per the need.
We will learn more in detail about this in our module about monitoring.
Oral Hypoglycemic drugs
The oral hypoglycemic drugs are effective in Type 2 DM. They are to be prescribed in low dosages, to begin with. The dose of the drug is increased as per the need. A single drug may serve the purpose or if not sufficient drugs may be given in combinations. The selection of a particular drug is based on the patient’s sugar reports and accompanying health conditions.
The commonly used drugs to treat Type 2DM
Metformin
Metformin is the first-line treatment. The mode of action is not yet clearly understood.
It reduces hepatic glucose formation and increases tissue uptake of glucose.
Bad taste, gastrointestinal disturbances, and lactic acidosis are side effects.
But in most patients, it is well tolerated. It is contraindicated when a patient has high serum creatinine values.
Sulfonylureas
They improve the function of beta cells.
The type of drugs under this heading are:
Tolbutamide, Chlorpropamide, Tolazamide, Glyburide, Glimepride, Glipizide,
Gliclazide, etc.
They too cause Gastrointestinal disturbances, hypoglycemia,
and also, have a Disulfiram-like effect.
(They cause nausea after alcohol intake)
Glitazones/Thizolidinediones
Pioglitazone and Rosilglitazone
They increase glucose uptake in tissues.
They have hepatotoxicity and are unsafe for the heart.
Alpha Glucosidase inhibitors
Acarbose, Miglitol
They block the conversion of disaccharides to monosaccharides by blocking the enzyme glucosidase in epithelial cells of the small intestine. Hence reduce the absorption of glucose into the blood.
Indigestion, flatulence, and diarrhea are side effects.
GLP1 Analogs: exenatide and Amylin Analogs: Pramlintide
They increase the secretion of insulin and decrease the secretion of glucagon.
They can cause pancreatitis due to continuous overstimulation of beta cells.
DPP 4 Inhibitors/ Gliptins
Sitagliptin, Vildagliptin, Teneligliptin, Linagliptin, etc.
These drugs come into action only when there is some food intake. They increase the duration of action of incretins secreted by the intestinal cells by inhibiting the enzyme DPP 4. This means they will reduce the glucose only when there is glucose intake. So they do not cause hypoglycemia and are safer drugs. At present they are a bit expensive. But these newer drugs are day by day becoming part of the prescription for Type 2DM.
Headache, Nasopharyngitis, and pancreatitis are side effects.
The dose has to be reduced in renal insufficiency. Safety in the pregnancy and lactating period is not yet established.
For extra reading please see the web page below.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2846464/?report=reader
Sodium-glucose co-transporter-2 (SGLT2) inhibitors
Dapagliflozin, Empagliflozin etc.
These drugs increase the excretion of glucose by inhibiting glucose reabsorption (which happens physiologically otherwise in renal tubules.)
But due to increased glucose in the urine, they cause polyuria, fungal infections in the urethra and around, and weight loss.
It is not at all advised in Type 1 DM.
To know more about these drugs, their dosages, the prescription details, please go through the webpage/book below.
https://www.ncbi.nlm.nih.gov/books/NBK482386/#_ncbi_dlg_citbx_NBK482386
Module 1 The Disease: Hypertension: Diagnosis
Hypertension
The word hypertension is used to denote increased blood pressure. Sometimes people call it by a short form as high BP. BP is blood pressure. Even patients know now that the BP should not go high as it will lead to a cerebral stroke or a heart attack. The incidence of such events is very common. People have started accepting these attacks as a new normal of life. But awareness about hypertension among people is increasing now. They ask doctors to check their BP quite often. Some doctors do keep watch on the blood pressure of their patients without being asked for it.
What is blood pressure?
We can imagine how amazing the design of our bodies is. The heart the size of a fist pumps the blood all through the six feet tall body and that too through the densely packed tissue. Nearly eighty such cycles in a minute and with no interruption in the entire life.
When blood is pushed through the arteries it has to have some pressure as any fluid flowing through an elastic pipe will have. We often see it when a gardener is watering plants or in a servicing center while washing a car. The forceful water is as energetic as an arrow. The water pump provides that energy. The heart in our body works similarly and gives energy to blood flow with rhythmic contractions. Blood carries nutrients and oxygen to every cell in the body. This process is known as perfusion. So to make it simple blood pressure is an essential function of the cardiovascular system that helps the body with the perfusion of tissues.
When an elastic rubber pipe carrying water is punctured by a pointed object what we get to see is a fountain. The height of the fountain is directly proportional to the pressure of the water flowing through. As a doctor, we witness a sprinkle of blood when a patient is brought with an arterial wound. That is not the case when the vein is injured. Blood simply oozes out when a vein is injured. That is because the blood in the artery flows with a higher pressure than the blood in the vein.
The fluid in the pipe exerts pressure on its wall and it is at a right angle to the wall of the pipe.
Similarly, our blood in the artery exerts pressure on its wall. And that can be measured and studied. The blood pressure of every artery will be different because they have different diameters, different types of walls, and are at different distances from the heart. So blood pressure depends on many factors. The blood poured into the artery by the heart also matters. We call it cardiac output. The amount of blood in the artery depends on the blood volume. Sometimes in dehydration or in hemorrhagic shock, the blood volume is depleted. Blood pressure falls automatically. Tissue perfusion reduces and the person goes in shock. Shock is a medical emergency and requires immediate action.
Definition of hypertension (HTN)
Hypertension is elevated blood pressure; systolic blood pressure(SBP) ≥ 140 mm Hg and /or Diastolic blood pressure (DBP) ≥ 90 mm Hg |
Primary hypertension
Hypertension with no definable cause is termed primary or essential hypertension.
Secondary hypertension
Hypertension caused by a specific organ or metabolic defect is termed secondary hypertension.
Classification of hypertension
Category | SBP/DBP mm of Hg |
Normal | <130/85 |
High Normal | 130-139 or 85 -89 |
Stage 1 hypertension | 140-159 or 90 -99 |
Stage 2 hypertension | 160-179 or 100-109 |
Stage 3 hypertension | >180 or 110 |
Grade 1 Isolated systolic hypertension | 140-159 and <90 |
Grade 2 Isolated systolic hypertension | >160 and <90 |
Evaluation of the patient with hypertension
The patient who is having elevated blood pressure is to be investigated to find out the cause of hypertension. That is to look for the secondary cause if any. In secondary hypertension, if the cause is treatable, patients need not take the life-long antihypertensive drugs.
Diagnostic tests in a patient with hypertension
ECG: to rule out cardiac complications and also for basal
Urinalysis: to rule out renal impairment
Electrolytes: to see levels of Sodium, potassium, and chlorides
Creatinine, BUN: to judge renal functions
CBC: to rule out anemia, infections, etc.
Fasting glucose: to rule out diabetes
Cholesterol: to rule out dyslipidemia
Chest X-Ray: to rule out heart enlargement, and lung pathologies.
Why is controlling hypertension important?
HTN is the most important risk factor for premature cardiovascular disease.
More common than tobacco smoking, dyslipidemia, and diabetes.
HTN is a cause behind 54% of strokes and 47% of ischemic heart disease events globally.
10-12% reduction in systolic blood pressure and 5-6% reduction in diastolic blood pressure can reduce 38% of strokes and 16% of coronary events.
End organ damages like retinopathies( Retina is an inner layer of the eyeball) and renal failures are the results of longstanding uncontrolled hypertension.
Module 1 The Disease: Hypertension: Treatment
Treatment of hypertension
Lifestyle changes
Diet, physical activity, and stress-free living help a lot. Weight reduction, keeping calories balanced, and regular exercises keep you fit.
Eat healthy food
Limit salt intake
Physical activity
Good to avoid alcohol
Do not smoke
Manage stress
Drug treatment
Antihypertensive drugs are available and should be used to bring the blood pressure in a normal acceptable range in every patient. There are many drugs and they have different modes of action. We have to select a particular drug according to the age of the patient, grade of hypertension, and any other disease the patient might be suffering from.
The commonly used drugs are from the following class of antihypertensive drugs. They are given in small doses, to begin with. Blood pressure is measured repeatedly and the dose is titrated. The doctor treating the patient has to consider many factors to get the right drug in the correct required dosage.
The grade and response of blood pressure are taken into account. A combination of drugs is tried to achieve the preferred blood pressure level.
Thiazide diuretics:
Examples: hydrochlorothiazide, chlorthalidone, Indapamide, Metolazone, chlorothiazide, Amiloride -
- Preferred in Heart failure, Elderly patients, Systolic hypertension
- contraindications: Gout, Dyslipidemia
Calcium channel blockers:
- Amlodipine, Cilnidipine,Diltiazem, Nifedipine, Verapamil, Benidipine, Efonidipine
- Preferred in Metabolic syndrome, Angina, Elderly, Systolic hypertension, Diabetes
Contraindications: Verapamil or Diltiazem not to be given in Heart block, and congestive HF
ACE (angiotensin-converting enzyme) inhibitors.
Examples: Enalapril, Lisinopril, Ramipril, Perindopril
Preferred in :
Metabolic syndrome, Heart failure, Left ventricular dysfunction, Post myocardial infarction, Proteinuria
Contraindications: Pregnancy, Lactation, Bilateral renal artery stenosis, Hyperkalemia, Renal failure
Angiotensin II receptor blockers.
Eexamples: Losartan, Candesartan, Valsartan, Irbesartan, Telmisartan, Olmesartan, Azilsartan
Preferred in:
Metabolic syndrome, Diabetes mellitus, Proteinuria, Left ventricular dysfunction,
ACEi induced cough
- Contraindications:
Pregnancy, Lactation, Hyperkalemia, Renal failure
Beta-blockers.
Examples: Metoprolol, Bisoprolol, Nebivolol
- Preferred in Angina, Post MI( Myocardial Infarction), Tachyarrhythmia, Heart Failure
Contraindications: Heart block, Dyslipidemia, Physically active, Peripheral vascular disease,
Elderly, Asthma, COPD(chronic obstructive pulmonary disease)
Alpha-Blockers
Examples: Doxazosin, Prazosin
- Preferred in Prostatic hypertrophy, Chronic Kidney Disease
- Contraindications: Orthostatic hypotension, Congestive Heart failure
Centrally acting drugs
Alpha methyldopa
- preferred in pregnancy
- Contraindications: Liver disease
Clonidine
- Preferred in Resistant hypertension
Contraindications: pregnancy and lactation
Hydralazine
- Preferred in Pregnancy, Resistant Hypertension
- Contraindication: Coronary artery disease
Module 2 The patient: Your role
Your role
As we have seen, people with diabetes and hypertension are mostly asymptomatic and many do not seek treatment nor do they visit the doctor. People need screening tests to know whether they have such types of illnesses. So we use this term patient here even for those who are suspected to have high levels of blood sugar, blood pressure, or blood lipids. One who is having prediabetes is on the edge of the disease. S/he is a potential patient and needs repeat examinations. The same is true for hypertension.
So when we use the term patient in this course it is a person who needs care for these diseases. The care may be a preventive measure. Screening tests are also part of patient care. Actually, it is care taken to reduce the number of patients!
Since both diabetes and hypertension affect every organ in the body, and there are so many aspects of studying these diseases; it is difficult to cover the subject in this short course. But you will get whatever you need to know from the internet nowadays.
It is difficult for you to remember all the drugs and details of their indications and contraindications. The information summarised in short here is just to get the idea of it. You can use it as a ready reference when needed.
The medical terminology is not easy to get familiar with within this short time. But with the time you spend with these words, you will find them simple and easier to use.
Your role can be explained shortly as follows
- To help in monitoring the disease.
- To visit the patient frequently and note down variables like blood pressure and blood glucose.
- To see if the patient is showing some symptoms which need some immediate attention by the doctor.
- To help patients in some emergency situations till they are taken to a doctor.
- To motivate the patient to take steps to control diabetes and hypertension.
- To guide the patient about proper diet and exercise.
- To help the patient to maintain proper medical records.
- To become a reliable friend of the patient and his family as such.
- To carry on as a medical guide/ voluntary health worker
- To gain information from resources to keep updated and be ready to use it when needed.
Module 2 The patient: A step towards relieving suffering
A step towards relieving suffering
Knowing about the disease is not enough. Only the patient will give you the unique experience to confirm your knowledge. To study medicine is science but to practice, it is an art.
We study the science behind the diseases and label patients as diabetic, hypertensive, etc.
But they are the individuals suffering. Every patient is an individual and requires separate attention. In real life when we meet them we need to get closer to them. We must assist them to get to know the disease they are facing. And assure them how they can get out of it or make it less troublesome.
Every patient has his/her own way to respond to the disease and the treatment. You are supposed to change your approach accordingly. Some patients can express their feelings, some can not. Some talk a lot, some are very quiet. Some can bear the pain, some will shout and cry loudly. But it is to be remembered that a sick person can not behave as one should behave otherwise. We should always keep calm and be thoughtful before any action.
What we plan to do is to help the patient to get better. In this course, we are limiting ourselves to monitoring diabetes and hypertension. That is we will measure blood pressure and blood sugar regularly. We have tried to understand the need of doing this in the last module. Mainly because both diabetes and hypertension are quite prevalent all over. And they bring about changes in our body so that we land into many acute and chronic troublesome conditions. We aim to prevent this from happening.
Module 2 The patient: Being a volunteer
We get joy and a sense of fulfillment when we help others. That is what volunteering is all about. A grown-up person with compassion and strong emotional and social intelligence will love to be a volunteer. It is found in one study that teenagers love to be a volunteer. They are curious, hard-working, and commit to the cause. They know that to grow is to know more about life. Life all around is a mix of all sorts of events and emotions. Illness is an unavoidable part of life. One has to face it as and when it comes.
A volunteer does things not as a job but as a new challenge. It is an opportunity to learn new skills. It is the way to gain confidence. It will teach you to communicate with others. Presenting the best of you to the community makes a difference. There is a possibility to develop the leader in you when you have a team of volunteers dedicated to a cause.
For science students who want to be a doctor, this course will be like premedical training. They can use their vacation period for this purpose. The idea to work with a doctor on a certain mission will be fun for them. They will get to meet patients and will have the opportunity to observe them. The history taking, physical examination, and investigations are the steps
In diagnosing any illness. To witness these steps with the doctor will be a great experience for these volunteer students.
Module 2 The patient: The first meeting
The first meeting
There are many possibilities for the introduction of a patient with the volunteer.
The volunteer is a patient itself.
The volunteer is from the same family and is related to the patient.
The volunteer stays in the neighborhood of the patient.
The volunteer will visit the patient from a distance regularly at a fixed time.
The volunteer will meet many patients in a health camp.
The volunteer devotes time to the hospitalized patients.
But in any case, the volunteer will require an introduction to the patient.
This will be the first meeting of this sort if the volunteer is not self or from the family.
The meeting place will be mostly the patient’s house. Daylight is preferred as the room will be well lit. The patient who is already diagnosed may have old reports/investigations which might guide you. It will be good to look at those papers carefully. But before that, you need to introduce yourself.
Introducing yourself is a skill to be learned. The meeting should of course begin with this self-introduction. Offering a greeting smile with the introduction will make further conversation easier. You will have to wait for the patient’s response to your presence, your smile. This will say a lot about the patient.
Did the patient smile back?
Is the patient comfortable?
Does the patient appear anxious, frightened, depressed?
Is the posture normal?
Is breathing comfortable?
Are the accompanying persons worried?
The conversation may not begin with the medical problems. It can be anything else trying to get closer to the patient. It need not be a pre-decided one but as the time suggests or the mood permits.
Though the volunteer is not a doctor, the patient should have the same kind of respect. The conversation therefore should be equally genuine and a serious one.
It is good to maintain that formality in the relationship. Let yourself be the listener. Let the patient say something. Allow the patient to begin the story; so you will know what the patient expects from you.
Your introduction, in the beginning, should include that you are there to help patients in monitoring diabetes and hypertension by taking repeated readings of blood sugar and blood pressure. And after a discussion with the doctor, may have to make certain changes in diet, exercise, and if needed in drugs too.
This will help in the fine-tuning of the control of both the diseases and it will give clues to doctors about the well-being of the patient in between the hospital or institutional visits. This also needs to be told in the very first meeting to the patient to clarify your role.
Module 2 The patient: The history
The history
The conversation with the patient may begin with the introduction and friendly smiles. Then one has to know certain details about the patient which have importance in total understanding of the patient and the disease.
When you note it regularly you have it on your records/notes which can be analyzed later on. It is to identify the patient first and not to mix findings with any other patients. Make proper entries carefully.
The name, age, sex, address, education, occupation, marital status are to be noted.
The information about smoking, alcohol intake, and diet history is a must. The patient should be allowed to speak freely about his complaints if s/he has any. The presenting complaint needs some further discussion to know the severity and other details. The complaint made by the patient is called a symptom. From the symptom, we can judge the organ or the system affected.
As we have seen, hypertension and diabetes both may not have any symptoms in the beginning stages. We may have to depend only on investigations to confirm the diagnosis.
But one reading is not enough for diagnosis and two or three high readings will be necessary. With any abnormal reading found you may have to report it to the doctor and know about the risk of complication. The patient may need a hospital visit after that. The doctor may make the decision as per the findings reported by you.
Here is a list of symptoms with their possible systems involvement.
General health | weight: over, under, Energy: fatigue, lassitude, Malaise Sleep: drowsiness, insomnia, disturbed sleep |
Upper Gastrointestinal tract | Pain: dull, burning, deep, spasmodic, Appetite: Reduced appetite, overeating Nausea, Vomiting, Hiccoughs, Fullness, flatulence, Waterbrash Dysphagia |
Lower Gastrointestinal tract | Diarrhea, Constipation, Pain: Dull, Acute, Colicky. Indigestion, Jaundice |
Genital system | Ulcerations, Itching, Dysfunctioning |
Cardiovascular system | Dyspnoea (breathlessness) Pain in the chest: precordial, jaw pain, hand pain, epigastric pain Choking sensation Palpitations, Cough, Edema |
Respiratory System | Cough, Sputum, Breathing difficulties, Wheeze, Chest pain |
Urinary system | Excessive/scanty amount, Increased /decreased frequency Pain: burning, dull, acute |
Nervous system | Stroke Seizure Headache Loss of sensations, Tingling, burning sensations Visual loss Hearing loss Loss of smell |
Skin | Infections, Allergies, pigmentations, |
Locomotor system | Cramps Wasting of muscles weakness/limping Joint pains |
Module 2 The patient: Small observations
The history obtained in short is not enough to conclude many times. But it can suggest to you an organ or a system involved. You are not going to do a complete examination as the doctor does but you can get information from small observations. It is good to know those points as they tell a lot about the patient’s health. This is not to make the diagnosis. But this will make a general assessment of the degree of illness.
Is the patient seriously ill and in need of immediate attention by the doctor?
How is the consciousness level?
How is the mental state?
Is there any pain in the chest that is making the patient restless?
Is the patient able to walk well?
Is the patient obese/ underweight/ normal?
Are the feet edematous?
Is there a wound/rash/eruptions anywhere on the skin?
Is the skin pale/ yellowish?
Is the patient having a high fever?
Module 2 The patient: Vital Signs
Vital signs are so-called because those are the signs of life. In medicine, in a patient's examination, vital signs have a special place. They are written at the beginning of the medical records. They give an immediate idea about the condition of the patient. What are these signs?
Temperature
Pulse
Respiration
Blood pressure
We need to know about these if we have to describe the health of the patient to someone else. Or if we want to record the serial improvement or deterioration in a patient's health.
The record of vital signs can tell you a lot about the patient. The normalcy of these signs will assure you about the general condition of the patient. And deviation of any of these signs from the normal will indicate the illness.
Body temperature:
Everybody knows about the use of a thermometer. We used mercury thermometers till now. We have seen people using digital thermometers too. And now with COVID-19, we are used to seeing the no-touch infrared thermometers.
Whatever be the instrument we must know that the normal body temperature is around 370 celsius /98.60 Fahrenheit. Everyone might have a small variation of this normal is also true. A temperature above 99.50 F is to be considered as a fever.
There are many causes for the patient to have a fever. Infections, inflammation, tissue necrosis, malignancy are common causes of fever. Fever is a common symptom that alerts the patient about the illness.
In simple terms, the patient can have a clear cause like respiratory infection, diarrhea, an infected wound, an abscess somewhere, etc. The patient’s fever may not have a clear explanation. We need to investigate such patients. Diabetes patients are more prone to have infections. We should immediately inform the doctor. Fever is to be seen and looked after by the doctor.
If the fever is high, more than 104 degrees Fahrenheit, the patient needs to be given antipyretic medicine like Acetaminophen/ paracetamol 500 mg stat (immediate) and may need sponging with water.
Pulse:
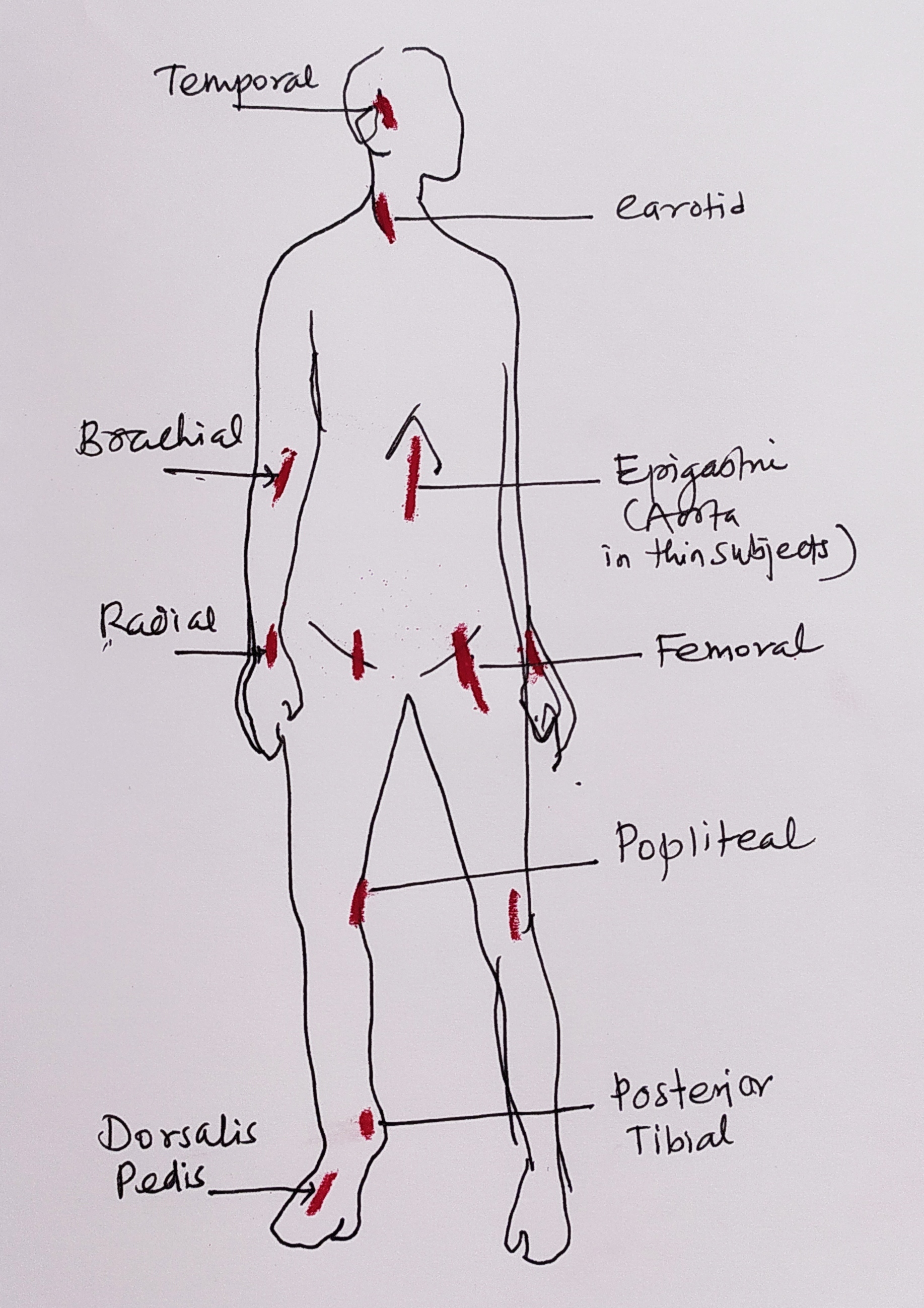
Pulse is like a wave that travels along the arteries. It is the result of the left ventricle pushing the blood in an aorta to travel through the other arteries with every contraction. The quality of that wave depends also on the elasticity of the arterial wall.
Pulse can be felt in any of the accessible arteries. Usually, the pulse a clinician feels is of the radial artery at the wrist. It is felt with the fingers by lightly pressing the radial artery on the plain radial bone below.
What we feel is mostly the rate, rhythm, and volume of the pulse. The normal pulse is from 55 to 100 beats per minute(bpm). Below 55 bpm is called bradycardia and above 100 bpm is called tachycardia. Changes in the rhythm are a big topic. We will not discuss that here but will just remember that loss in the rhythmic contraction of the heart causes many arrhythmias. And these are due to the defects in the electrical conduction patterns of the heart.
Respiration:
The newborn baby has a respiratory rate (RR) of 44 cycles per minute. It goes on decreasing as we grow up. Adults have a respiratory rate of 14-18 cycles per minute. Increased respiratory rate is tachypnoea. The decrease is bradypnoea.
Respiratory rate is counted as cycles of breathing (inhalation and exhalation) in a minute. It is a skill to count the respiratory rate as it requires the diversion of the patient’s attention. If the patient is conscious about respiration, it affects the normal pattern of breathing.
Tachypnoea is found when the patient has exertion, fear, fever, heart weakness, pain, lung diseases like pneumonia, embolism, pneumothorax. RR increases in anemia, hyperthyroidism.
Bradypnoea is found in the intoxication of CNS depressant drugs, in the condition of uremia, and also when there is raised intracranial pressure.
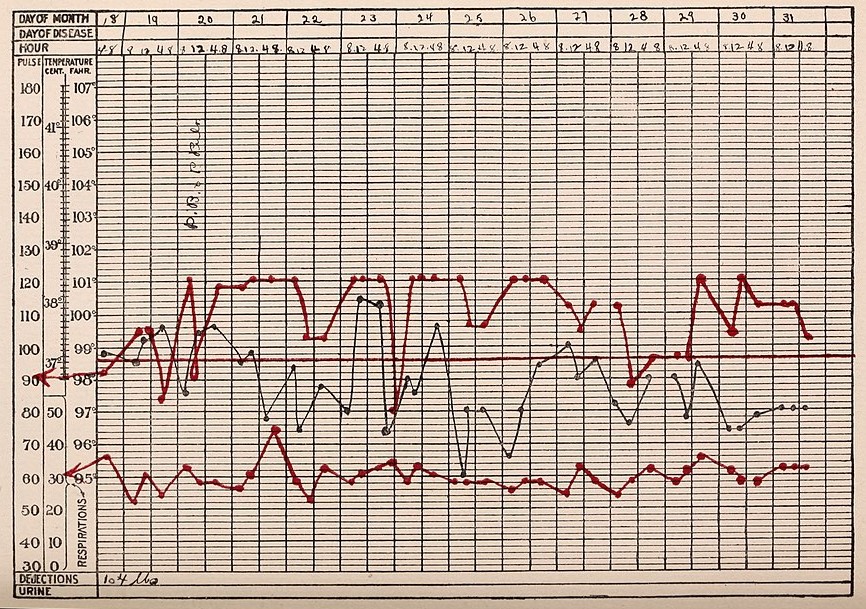
The image below is from old files and gives an idea about TPR charts.
If you see a file of an admitted patient in any hospital the first thing you notice is this sort of graph which is
Temperature, Pulse, and Respiratory rate chart. This gives an idea about the health of the patient at a glance.
This is mostly maintained by the nursing staff of the ward. Accurate and timely entries in this graph are must.
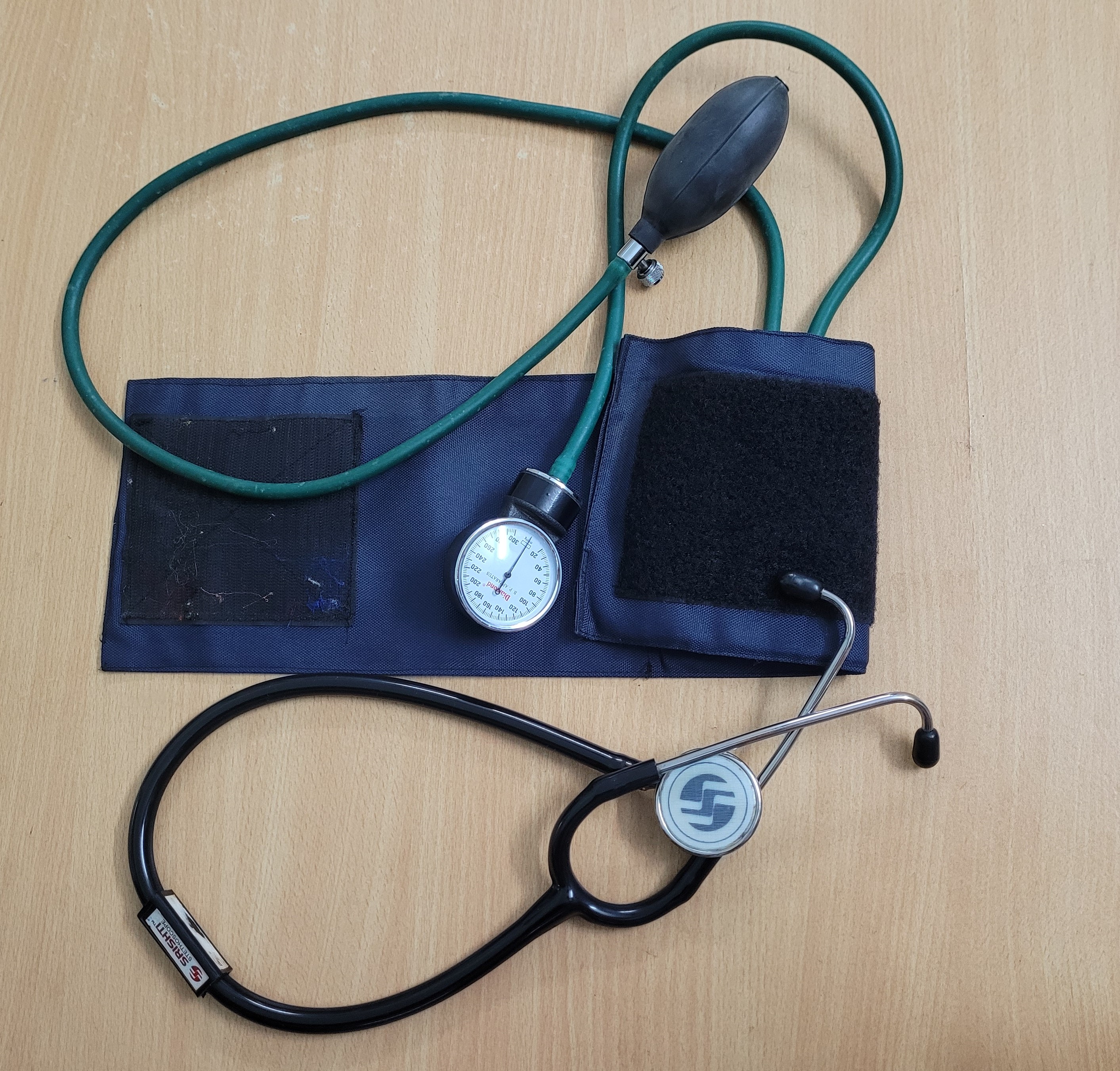
Blood pressure:
We have already discussed what blood pressure is. Here we will see how we check blood pressure. There are two types of blood pressure apparatus available. One is a manual type and the other is automatic. Manual apparatus requires a stethoscope to auscultate and a pumping balloon to inflate air in the cuff. It has either a mercury column or a dial calibrated to give readings. The electronic types of equipment give readings on screen and do not need a balloon to inflate air. They have an inbuilt motor/pump to push air.
We will see some important precautions at the time of measuring the blood pressure.
The arm cuff used in BP measurement should be wide enough to reduce the error.
The patient should be at rest for ten minutes before measuring ideally.
Feel the brachial and/or radial artery pulse before inflating the air into the cuff.
The patient can be sitting or in a lying down supine position.
When you inflate the air in the cuff, at one point you will notice the disappearance of the pulse. Inflate further for 30 mm above that point. (This you can judge with mercury or dial sphygmomanometer. In digital instruments, we do not see the column but the numbers come on the screen. There you don’t have to feel the pulse too. The readings follow as you start deflating the air in the cuff.)
To get systolic and diastolic readings we have to start deflating the air in the cuff slowly with the stethoscope put at the cubital fossa on the brachial artery. Vibrations of the artery make sounds known as Kortkoff sounds.
The point where the sounds start is the systolic blood pressure.
The point at which the sounds start fading and disappear is the diastolic blood pressure.
In some people, Korotkoff sounds do not disappear but continue till zero. Then the point at which the sounds start fading is taken as diastolic blood pressure.
Whatever be the instrument used the blood pressure is always written as Systolic blood pressure/ Diastolic blood pressure mm of Hg. We say ‘mm of Hg’ as a millimeter of mercury. For example, 120/80 mm of Hg means systolic BP is 120 diastolic BP is 80 mm of mercury.
Oxygen saturation level
https://youtu.be/ifnGCz0cgvs
This investigation has suddenly become an important one in this pandemic of COVID-19. Doctors are advising patients to have a pulse-oximeter reading frequently and report it to them. This reading gives an idea of the severity of the disease and the decision of treating the patient varies accordingly.
Pulse-oximeter is a small machine previously used mainly by chest physicians or in intensive care units. It is a piece of thumb-size clip-like equipment that runs on a battery. There is a small screen for the display of results.
Pulse-oximeter is applied to the fingertip and we can see the pulse and oxygen saturation level on the screen within a few seconds. Such a quick test and easy to use for anyone. Oxygen saturation of more than 95% is considered normal. 92% and below are the patients who will require oxygen to correct their hypoxemia/hypoxia. Low levels of oxygen saturation indicate less supply of oxygen to tissues, that is reduced tissue perfusion. It is a life-threatening condition and is not to be ignored.
But some patients with COPD (chronic obstructive pulmonary disease) may have low levels of saturation normally.
Will like to share here a TED lecture titled `Wireless future of medicine'. It is a magic world but not for all. What we are going to learn is simple
https://www.ted.com/talks/eric_topol_the_wireless_future_of_medicine
Module 2 The patient: Height, weight, body mass index(BMI), and waist-hip ratio
Height
Height is influenced by genetic and environmental factors. Height goes on increasing from childhood to adolescence till maturity. Then it remains stable for years. But with some degenerating changes and in osteoporosis some reduction is seen. With the change in an erect posture, we do observe a reduction in height.
Height is measured from ground level to the topmost point on the scalp when a person is standing erect and bare feet. It is recorded in centimeters or feet and inches.
Bodyweight
Weight is an important variable and needs frequent measurements to assess and compare health status. In diabetes and hypertension weight needs constant attention. Having an extra burden of weight puts the physiological systems under stress. Obesity is a common medical condition nowadays. It is associated with Dyslipidemia, Type 2DM, hypertension, Cardiovascular diseases.
Alarming weight loss is also seen sometimes and needs investigations. It can be due to cancer, viral infection (such as CMV or HIV), gastroenteritis, parasite infection, depression, bowel diseases, and overactive thyroid (hyperthyroidism).
Measuring Weight: Each visit must include weight measurement as a routine. Electronic scale gives accurate and sensitive readings. It is lightweight and portable too. Weight is recorded in pounds or kilograms.
Body mass index(BMI)
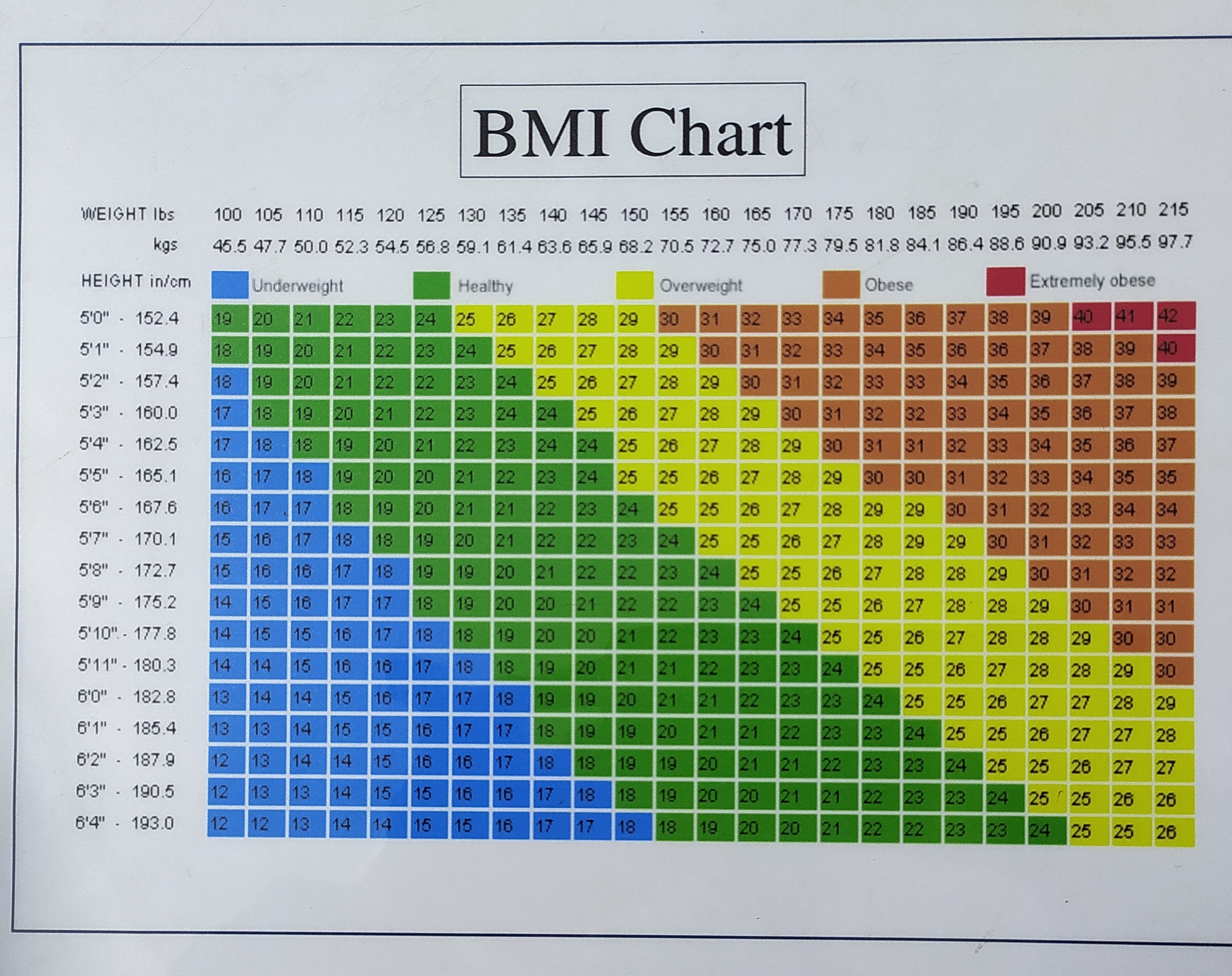
BMI is a ratio of Weight in Kilograms to the square of the height in meters. So the unit of BMI is kg/m². BMI is called the Quetelet index. BMI indicates risks of diseases and is used to set goals in the treatment part of both diabetes and hypertension. Below is a short table that will help to interpret the BMI. Here weight reduction will help to get into the normal zone.
BMI calculations are clinically useful to set goals. Explaining the degree of obesity with BMI numbers to the patient becomes easier. Having a BMI chart handy is useful.
BMI | Interpretation |
<18.5 | Underweight |
18.5 to 25 | Normal |
>25 to 30 | Overweight |
>30 to 35 | Class 1 Obese |
>35 to 40 | Class 2 Obese |
>40 | Class 3 Obese |
Waist-hip ratio
Waist circumference tends to increase in midlife. This is mostly due to increased fat in the omentum. This is the age when Type 2DM starts. So this adiposity is found to have a connection with insulin resistance.
The waist-hip ratio is the ratio of body circumference at the waist and hip of a person.
The normal ratio for males is below 0.9 and for females, it is less than 1.
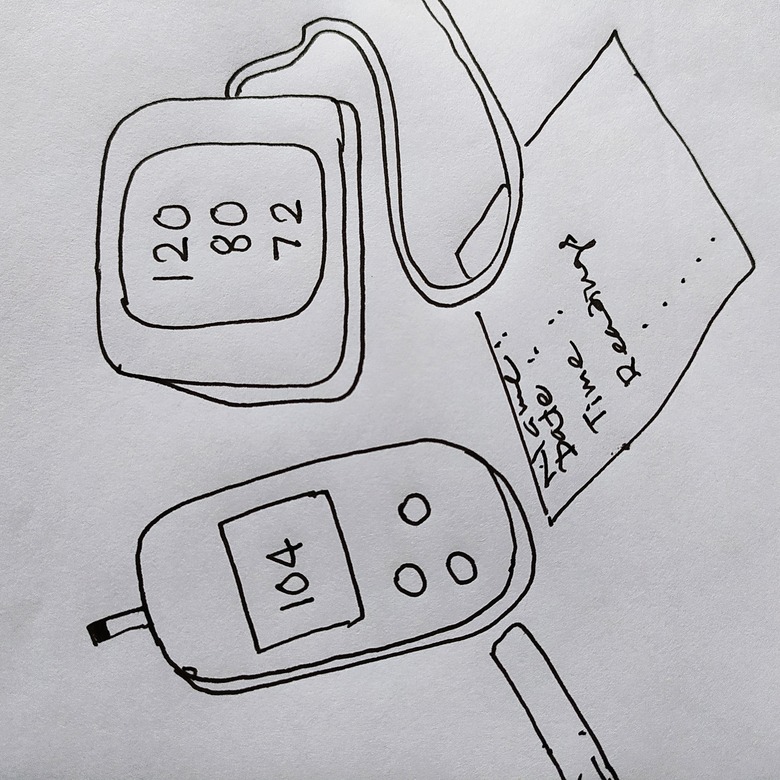
Module 2 The patient: Blood glucose test by the glucometer
Glucometers are handy and are about the same size as that of a mobile phone or smaller than that. They are battery-operated mostly. They have a notch where a strip is to be inserted. Strips have a mark or arrow to tell you which side goes in the notch. The other end has the part where the blood drop is put.
A simple one-minute test is easy to do and gives us a quick reading of blood glucose. It shows the glucose concentration in blood in milligrams of glucose per 100 ml of blood. This number appears on the screen when you perform the test as per the guidelines. Most glucometers give suggestions for the performer of the test on their screens. The glucometer starts functioning with the introduction of a strip and stops with the removal of the strip.
The drop of blood is obtained by pricking a fingertip. It is a good practice to prick not in the center but on the sides of the finger. It is to avoid a prick to the tendon below. If injured it gets inflamed and will have pain for a longer time.
All aseptic precautions are to be taken. Cleaning your hands before doing the test is a must. And cleaning the fingertip of the patient should also be done. Cleaning with a spirit swab is avoided while doing a sugar test as it is possible that the reading might change due to alcohol. Spirit/ alcohol if used, we should wait till it dries out and then make a prick with the lancet.
You have to press the sterile cotton swab at the prick site for about a minute or two. This will stop the oozing of blood. Remember the blood-stained swab and the lancet has to be disposed of and treated like biomedical waste. Your doctor can guide you in this matter. Be careful not to get an accidental prick to you from that lancet. Such pricks do occur if you are not attentive enough.
(A video showing the test here.)
Module 2 The patient: Hypoglycemia
Measuring is one thing and knowing the meaning of the measurement is another thing. If you can not conclude the reading of blood pressure, blood sugar, or temperature then the result you get is just a number. It can not help the patient. So it becomes necessary to learn the meaning of those readings.
What if the patient has a low pulse rate? What If it is high? What may be the cause of the raised temperature? Is the respiration of 30 per minute normal? Is the blood pressure of 180/100 mm Hg acceptable? Such questions may arise in your mind. The reason we are trying to know more about our body functioning is this. It is good if you know which readings are acceptable and which need immediate attention or consultation with the doctor.
Here we will learn more about abnormal test results and the steps we follow then.
Hypoglycemia
Blood glucose level is maintained in a range and many hormones and tissues play a role in this process. We have discussed it before being a part of the homeostasis. Hypoglycemia occurs when glucose utilization is increased and intake and production are decreased. Hormones like catecholamines are released to increase glucose. These increase sympathetic activity and cause symptoms like palpitations, sweating, anxiety, hunger, and tremors.
The common emergency faced by diabetic patients is hypoglycemia. Patients take drugs or insulin injections to reduce the raised blood sugar. But if they take a higher dose of the drug or the injection they can present with hypoglycemia. It can also result from a lower intake of diet or excessive exercise or due to accompanied illness like diarrhea or vomiting. Children with Type 1 DM also have hypoglycemia possibilities as they are playful and may miss a proper time for a meal.
Blood glucose below 70 mg/dL is considered hypoglycemia. A patient’s brain cells require glucose for functioning. If they are deprived of glucose we start getting many symptoms. It will have a different presentation for every patient. Many patients can learn to recognize these and with experience will consume a sweet and get to normal. But if they miss noticing they may become drowsy and their consciousness is affected.
Hypoglycemia may cause death if it is severe and prolonged.
Common symptoms of hypoglycemia
Palpitations due to increased heart rate.
Sweating
Anxiety
Hunger
Tremors
Headache
Confusion
Light-headedness
Irrelevant behavior
Slurring of speech
Visual disturbances
Seizures
Coma
Common causes of hypoglycemia
High dose of Insulin or Oral hypoglycemic drugs
Alcohol
Starvation
Some insulin-producing tumors
Treatment of Hypoglycemia
If the patient is conscious enough we should give him/her sugar to eat. Three to four teaspoonfuls of sugar in powder form or glucose powder should be given. Then check the blood sugar again after fifteen minutes. The patient is advised to take frequent small meals and necessary changes in drug and insulin dosages are to be done. It is to be discussed to remain watchful for symptoms of hypoglycemia next time.
If the patient is not conscious we can rub glucose in a paste form on buccal mucosa. It does raise the sugar level. Non-responding patients will need intravenous glucose. Either call the doctor for this or shift the patient to the hospital for further treatment.
How to avoid or prevent hypoglycemia
We need to educate the patient and the relatives about the condition of hypoglycemia and the need to report to the doctor as early as possible. They should be informed of dangerous complications of not recognizing and not treating hypoglycemia.
Diet, drug treatment, and exercise need proper planning.
Frequent blood glucose examinations tell us about the possibility of hypoglycemia in time.
Be prepared for hypoglycemia treatment
Every diabetic patient must carry a card mentioning that he or she is having diabetes. If he or she is found unconscious then people will know the cause of his unconsciousness from that card. The card should have that type of message for people and that a doctor needs to be informed. Details about contacting the doctor will be helpful for quick treatment.
It is useful to tell friends and other people who are related to the patient by means of work or so that the person has diabetes. The patient has to do this. There is no need to hide the condition of diabetes. Though the patient knows every symptom of hypoglycemia, in a confused state it is difficult for him to do the right things.
It is good to carry a kit containing sugar, fruits, biscuits, or chocolates by the patient when away from home.
Glucometers should be carried on a journey.
It is good if blood sugar is checked before and after any sports activity by the diabetic patient.
Module 2 The patient: Metabolic Syndrome
It is a newer term and relates to the disease complex as a result of the combination of Central/abdominal obesity and insulin resistance. It includes
High blood glucose
High blood pressure
Cardiovascular diseases
High triglycerides
High insulin levels in the blood.
It will be good to see if our patient fits into this complex disease combination. This is important because there the patient needs to be more alert about monitoring. The atherosclerotic changes in vessels need to be reversed by proper daily exercise and dietary changes.
Module 2 The patient: Keep an eye on eyes
Diabetes and the eye problems
You might observe the following eye problems in a diabetes patient
Stye: It is an infection on the eyelid at the base of an eyelash.
Early-onset of refractive error.
Glaucoma: Raised intraocular pressure. Presents with pain in the eye and redness. Can lead to blindness.
Diplopia: Double vision
Early-onset of cataract.
The retina changes: hemorrhage, degeneration.
Corneal abrasion and ulceration
Module 2 The patient: Diabetic foot
Diabetes affects small blood vessels and peripheral nerves badly. Many people experience these changes as the disease progresses. Burning sensation or tingling and numbness are common symptoms. Patients have total loss of sensation sometimes. This is a difficult time and it becomes troublesome to walk or keep balance and stand on feet.
Patients have injuries on soles and they don't know it. Injuries get infected. Bacteria enter cells around the wound and there is swelling and redness. It is called cellulitis. If not intervened by the effective treatment it's a serious condition that can lead to gangrene.
Gangrene is necrosis. This means it is the death of the tissue affected. The necrosed part has to be removed and hence sometimes we see diabetic patients who have to get an amputation done of the affected part of the leg.
Is diabetic foot preventable?
Proper care can prevent a diabetic foot. It is monitoring diabetes well which prevents peripheral neuritis. Regular self-examination of the foot done by the patient is advised. A mirror is to be used to see soles. Using soft footwear can prevent injuries. Early identification of the wound and careful treatment of the wound with frequent dressings and antibiotics is a must.
Every patient should learn wound care. Patients should always avoid tobacco and alcohol. Because they both speed up the process of neuritis. Since the wound is painless patients do not take rest or proper care. If they do not take enough antibiotics the wounds do not heal in time.
Module 3 The monitoring: Readings: monitoring
Monitoring Diabetes and hypertension is not episodic work but a daily routine for the patient. We can say that monitoring is the treatment of these diseases. Since the complete cure is not possible we have to just carry on with monitoring. Even for those who claim the reversal of the disease, how can we be sure about that unless we do check patients repeatedly.
One who has such a kind of illness can not just neglect the care. The patient should always keep in mind that monitoring is the only way to know how well the treatment is working. By doing the blood glucose test frequently you can judge the food you eat, the exercise you do, and the drug treatment you follow is appropriate or not.
You can monitor blood glucose and /or blood pressure when you know the level you are aiming for. When you do it regularly you are able to interpret the result and connect them to food, exercise, and drugs. You can make changes in these three modes of treatment and achieve the glucose and blood pressure levels in the most effective way.
In the past, we used to test urine and monitor diabetes. But that was very crude and not that sensitive. But with glucometers, it has become easier and more accurate to do so now. A negative test in urine examination will indicate that the blood glucose can be anything below 180 mg/dL. It can be reading of hypoglycemia too i.e. below 70 mg/dL. So a blood glucose test really helps you to know the exact status at that particular time.
Monitoring glucose is good for the long-term aim of preventing organ damages. But it is sometimes essential to monitor it strictly in some situations.
- When a diabetic child or an adult takes part in any sports activity it is necessary to make sure that hypoglycemia does not occur in the middle of the game.
The same is the case with a diabetic driver on a long drive. Hypoglycemia is to be avoided as it will interact with alertness while driving.
Diabetes management in pregnancy is also very strict. Needs frequent checkings to maintain blood glucose in the normal range. High blood glucose levels have an adverse effect on a baby’s development.
Alcohol intake in a diabetic always is a risky thing to do. Possible hypoglycemia is to be avoided by doing frequent blood glucose tests.
At the time of illness, blood glucose levels become unpredictable. It becomes mandatory to check it and monitor it.
Before any surgery, we need to get the blood glucose in a normal range. A planned surgery like cataract surgery has good results only when the blood glucose is well controlled.
When any new drug is started or a dose of insulin is changed we need to check it again and again.
If the daily routine changes due to some reason we need to do blood glucose tests. It can be a change in a job you do or the hours of working that change. These changes can change blood glucose too.
When there is concomitant use of steroids or any new drug which has a possible effect on blood glucose level it is a must to check and see if it has changed. We can adjust our antidiabetic drugs accordingly.
In this covid pandemic glycemic control is a must. Diabetes with Covid-19 is found to be a difficult combination to manage. Monitoring blood glucose definitely helps in a good recovery.
Module 3 The monitoring: Recordings: Maintaining records
Keeping a diary is a good habit for everyone. It becomes a must for a person with diabetes and hypertension. The date, time, blood pressure, and glucose test results with other relevant notes will make them useful in the total management. If the patients make it a habit to enter the drugs taken and the dosages also it will be complete documentation. Diet and activity records along with these will help to see the relationship between the efforts taken to keep the control and the results obtained.
Good records make it easy for the patient and the doctor to see the course of the disease well. They can judge the progress just by looking at well-maintained records. It is a doctor who has to stress the importance of keeping the readings recorded properly and in chronological order. It is good if the doctor has all the records with him/her too. Digitization has made it simple to trace and keep records up to date.
We as a mediator or volunteer should play an important role to help the patient maintain their diary/records well. We should guide the patient about the preparation before their visit to the doctor. The patient should know that the doctor expects to see reports, medicines, and dosages. The doctor should get the correct idea of symptoms, diet, physical activities.
With the records in hand, we can actually see a pattern of blood glucose or blood pressure over a definite period and decide the action we need to take. For example, avoiding particular food or to become more active, or changing the drug/insulin dosages. But while doing any major changes we need to consult our doctor
| Diabetes registry proforma |
Name of the volunteer/reporter:
Date:
Time:
Place:
Description: | Details: | Fill in: |
Name of the patient: | ||
Address | ||
Age | ||
Sex | ||
Occupation | ||
Blood glucose today | ||
Age of onset of diabetes | ||
Medicines | oral or Insulin or both | |
Height | cm | |
Weight | kg | |
Abdominal girth | cm | |
Known complications & associated conditions | (tick mark complications/conditions) | |
hypertension | ||
hyperlipidemia | ||
ischemic heart disease | ||
peripheral vascular disease | ||
diabetic foot/amputation | ||
retinopathy | ||
nephropathy | ||
neuropathy | ||
Educational status | illiterate or primary education or secondary education or higher | |
Economical status | poor or middle class or high income |
Module 3 The monitoring: Requesting: Motivating the patient
Patients who are well educated and can afford to visit consultants frequently probably do not need your service. They will manage their illness well. But those who are not educated enough and are poor will require your voluntary work.
Diabetes and hypertension are different from other short-term illnesses. Many people fail to understand this. They want to recover fast. They have a tendency to ignore that they have an illness. This is very common and a natural human behavior. We do not want to see ourselves in any difficult situation. We just try to neglect the need to know the truth, a bitter truth.
People may not like you when you remind them of their illness. They will keep you away. Then it becomes more difficult to deal with them. Our first job is to make them know they need to monitor their disease. You can explain it step by step and not all at a time. With an easy, casual, and friendly approach we should demonstrate that it is an easy task to keep watch on the disease. Though you know many theoretical possibilities of disease progression you must not tell them to the patient on the very first day. This you can achieve as and when the need arises.
Never ever should a patient feel like rejecting the help you are providing. Understand the currents of thoughts the patients have about you and the disease. Observe their expressions and words. It will help you to do that. Make sure that your words or actions will not hurt patients anytime.
There is a possibility that some patients may be very old and do not want to get treated. They may be living with depression. As such diabetes and hypertension can alter the mindset of the patients as a part of the pathology in the later stage of the disease. These patients may have memory problems and may not remember you sometimes. They may be bed-ridden and non-ambulatory. Remember they need you badly then.
Module 3 The monitoring: Resistance: Obstacles in monitoring
There are many obstacles in our way of monitoring diabetes and hypertension. We should identify these and try to find appropriate solutions to them. It is not going to be easy every time. When you know that you have chosen this work to change things then you will work on the ideas to make it happen. We will just try to list a few obstacles . We have to take them as a challenge, a part of our job
- The patient is ignorant/not worried about his/her high blood glucose or blood pressure levels.
The patient does not give you time to test.
The patient does not take medicines in time.
The patient does not follow the diet guidelines.
The patient is tired of doing tests.
The patient tries out illogical things as a part of the treatment.
There are family issues and quarrels that keep you worrying about.
The patient hides information about symptoms, drugs, etc.
Module 3 The monitoring: Referring: Informing the doctor in time
It is important to know when you should seek advice from a doctor. When you see some alarming symptoms you should not waste much time but ask the patient to get examined by the doctor.
If the hypoglycemia does not improve, it means if the blood glucose remains below 50 mg/dL even after giving plenty of glucose or food rich in carbohydrates. The patient might need intravenous administration of glucose that time.
If repeated blood tests for glucose show reading higher than 250 mg/dL. Definitely some change in the treatment is needed.
If the patient has a fever. Fever suggests infection. Diabetes with infection is quite not good for one's health. Fever needs to be properly diagnosed.
Any skin lesions with ulcer or abscess.
Non healing wounds.
Diminishing vision
Severe abdominal pain
If the patient has breathlessness
Module 3 The monitoring: Revisiting: Follow-ups
How frequently should you test the blood glucose and blood pressure is the question.
Some patients don't know the logic behind testing. They try to underestimate the need to do so. The common practice they follow is problem-oriented. They will get examined only if they have some problem. This is a big problem and their diabetes and hypertension remain unmonitored. There are chances that they will have uncontrolled blood glucose and blood pressure. So they are heading towards complications unknowingly.
One should decide the frequency of follow-ups just by test results. If the patient has abnormal test results then we need to do some corrective measures. We need to check again and again to see how effective our measures are. We may have to see it twice, thrice, or even more frequently in some cases. If the patient has learned to check it then it becomes easier. Self-monitoring of glucose and hypertension is best possiblething to have in managing the diseases.
For patients staying in villages and diagnosed with diabetes and hypertension, they should be followed up at least once a month if their previous readings are around normal levels. If they have high readings then they will need multiple testings. Titrating the dosages of drugs will have to be done depending upon the test results.
Module 3 The monitoring: Reminding: Guidance to the patient
Educating patients is a slow process. They can not grasp everything they need to know in one meeting. In each meeting, we should reserve some time to elevate the level of understanding of the patient about the disease. We need to explain the basis of the treatment and give stress on precautions to prevent complications.
Some common questions patients frequently ask or may want to ask are worth going through.
I would like to add a few possible answers here too.
Why did I get this disease?
-It is common nowadays. But it is to be controlled in time. Now since you have it you have to take proper care.
Will I get rid of this and live as before?
-Definitely. With some diet changes, the proper exercise you can control it. But it is learned from the experience so far that you can not ignore it. You have to keep a continuous watch on blood glucose levels, blood pressure and that is not difficult. We can do it. Not to worry. You can always live as before but with some supportive drug treatment.
Can I get some better treatment from another doctor?
-If your blood glucose is well under control and if you do not have symptoms of complications it is better to stick to one physician and monitor properly
How is the other patient in the neighborhood with diabetes not having any problem?
-No two people will have the same response to the treatment.
What will happen if I do not take any treatment for some days? Should I try doing that?
-It is not a wise decision. One should always take the treatment and stay safe.
Why should I continue the medicine if my reports are so normal now?
-Reports being normal is a good thing. But it is because of the treatment they are normal.
How can diabetes cause a heart problem?
If I am not eating sugar now, how do my reports show high blood sugar?
Is it necessary to tell people around me about my illness?
Should I attend the party and eat whatever they will serve or should I suggest to them about my dietary restrictions?
What if I get hypoglycemic on a journey?
Are ayurvedic medicines safer and better than allopathic or modern medicines?
It is an unending list and it will vary from patient to patient. But we need to study these probable questions and deal accordingly. If you know the facts then you can find better words to guide.
The most important thought to remember is never ever to create fear in a patient's mind. Even if you know the bad prognosis you should always speak about hope. Hope keeps people going. Kind words with simple helpful suggestions will make a huge difference.
Module 3 The monitoring: Restrictions: Know your limitations as a volunteer
The volunteer is like a member of the family trying to help another member of the family. The readings of blood glucose and blood pressure are important to decide the prognosis or fate of diabetes and hypertension. Hence timely measurement is going to be a great help for the patient.
But when I thought about this course, I had many questions in mind. Those were mostly about how the patients will cooperate with these volunteers? If the person examining is not qualified in the subject, how well his/her opinion will be honored? What if some decision-making is not helpful for the patient? What if any emergency is beyond the volunteer’s capacity?
These are all very important questions and they need to be answered well before we proceed further to make this course work in reality. To make volunteers capable to face these questions is quite a necessary step.
If the volunteer knows his/her limitations the answer is simple. We need to work with the patient after proper consent. The patient should know well that measuring blood pressure and blood glucose is the only responsibility of the volunteer. The volunteer is there to alarm and suggest further treatment.
The readings obtained by the volunteer are to be finally analyzed by the doctor. The ultimate decision is with the doctor and not the volunteer.
If there is any confusion about readings the patient is free to visit a doctor for further check-up.
I have no doubt about the role of the volunteer in the management of these patients. But the volunteers should never try to replace a doctor at any time. |
Module 3 The monitoring: Risk reduction: the tight control
Body processes are not predictable for us sometimes. The way some cases deteriorate is beyond our understanding.
Infection is a big threat to diabetic patients
We have witnessed in the recent pandemic of covid19 how some people having diabetes and hypertension as comorbidity collapsed suddenly. We could not help them survive. They are easy targets it seems. Let that be HIV, tuberculosis, Urinary tract infections, types of pneumonia or skin and soft tissue infections. The doctor has to be very prompt and very much attentive if the patient is a diabetic. The volunteer should also keep this in mind about diabetes and infections. They are not to be taken lightly. Even a simple skin wound may turn into severe complications if diabetes is not under control. The present situation of fungal infections is worrisome.
Any surgical procedure may it be a tooth extraction requires fine control over blood glucose and blood pressure.
The same is true with cataract surgeries and all other surgeries. The idea of continuous monitoring is the best strategy to follow.
Diabetes and hypertension together are bad for the heart
The risk of a cardiac event is manifolds if the patient has diabetes or hypertension, studies have shown.
Some unpredictability is always experienced in these vascular diseases. Many such sudden incidents make us wonder. We have no answers really. But to keep on thinking whether something done in time could have prevented these from happening. But those are afterthoughts.
We still are not able to cope up with these shocking events and need to concentrate on monitoring well.
Blindness is preventable
Diabetic retinopathy is a complication that leads to loss of vision. But it can be prevented with early diagnosis and good glycemic control of diabetes. It is proved that microvascular complications can be postponed with good monitoring of blood glucose.
Hemodialysis and renal transplants are not the answers
When capillaries of kidneys get affected due to diabetes we say it is diabetic nephropathy. Uncontrolled diabetes and hypertension both cause end-stage renal disease. This is so common complication and the patient lands up with the thrice a week hemodialysis or kidney transplant as a last resort to survive. It is so expensive mode of treatment and many poor people can not just receive it. Monitoring can avoid the need for hemodialysis if applied well at the beginning of the disease.
Peripheral neuropathy leading to gangrene and amputations
The pain is felt due to the sensory nerves doing their work. Touch, temperature, and vibration sense make us responsive. If the nerve function gets affected we start getting some altered sensations. We get unbearable pain and burning or sometimes we can not feel the pain or even the touch. This we call peripheral neuropathy.
Neuropathy can lead to non-healing wounds, cellulitis, gangrene. The patient may require amputation to survive.
The studies done have come to conclusions supporting that the risk of complications gets reduced with the tight control over diabetes and hypertension. This finding is a basis behind the monitoring.